


In the healthcare, Medical credentialing solution is an integral part of healthcare in the United States. It is when a practicing physician’s qualifications are verified to certify that he or she is able to provide medical services. Insurance companies carry out the process of health care credentialing to attest that a provider is authorized to provide care to patients who are members of the insurance payer’s health plans. Most, if not all health insurance companies require this process.
Credentialing in healthcare is used to validate a physician’s education, experience, certifications, license, history, and so forth. Unsurprisingly, the entire workflow around credentialing is highly inefficient and time-consuming, not to mention, prone to errors. It involves a lot of paperwork and an elaborate procedure of processing and finalizing a provider. It goes without saying that the entire process is bound to incur its own expenses.
That is when a credential management system can help insurers accelerate the credentialing process, and also enable providers to begin offering services faster.
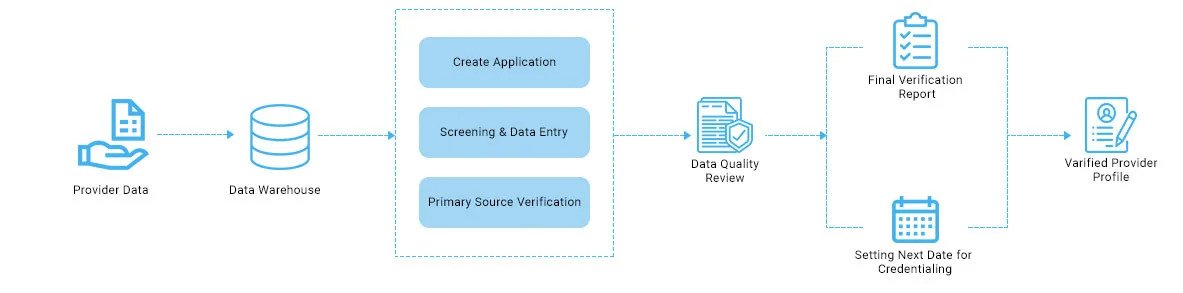
When a payer organization wants to include a provider into its network, it collects the necessary data from the doctor, develops a roadmap for credentialing, verifies the data for its authenticity, manages the entire profile of that provider whilst validating his or her certificates. So, it should not come as a surprise that each of these activities requires its own workflows, dedicated staff, and organizational resources. As a result, this conventional way of doing things manually incurs greater overhead, not to mention having lots of room for errors.
But using a software solution to carry out credentialing in healthcare will automate most of the activities mentioned above. Furthermore, a software platform also digitizes many of the workflows involved. Consequently, automation and digitization together directly translate into greater efficiency and productivity of the entire process of credentialing. Additionally, since there is digitization, activities that previously needed physical documentation with pen and paper can now be done with some clicks. To sum it up, a smart solution for healthcare credentialing services not only speeds up the process, but also helps payer organizations reduce operational overhead, whilst also boosting productivity. The result is a win-win for payers as well as providers.
Some of the leading healthcare credentialing services also offer what’s called centralized credentialing. In this, multiple healthcare organizations, including large hospitals and smaller ambulatory care centers conduct the process of credentialing together. In other words, they share the cost and other resources that go into the process. Furthermore, the providers too don’t have to undergo the process multiple times, further improving the overall efficiency of credentialing. This goes a long way in improving the relationship between them and the administrative management at the hospitals. In addition to that, it also helps broaden the payer network faster, without too much investment into time or resources.
Medical credentialing is a process that every provider must undergo in order to get included in insurance payers’ networks. Smart, digital solutions for the entire procedure of medical credentialing go a long way in helping payers reduce overhead, improve operational efficiency and assist providers to get into payer networks.

















